 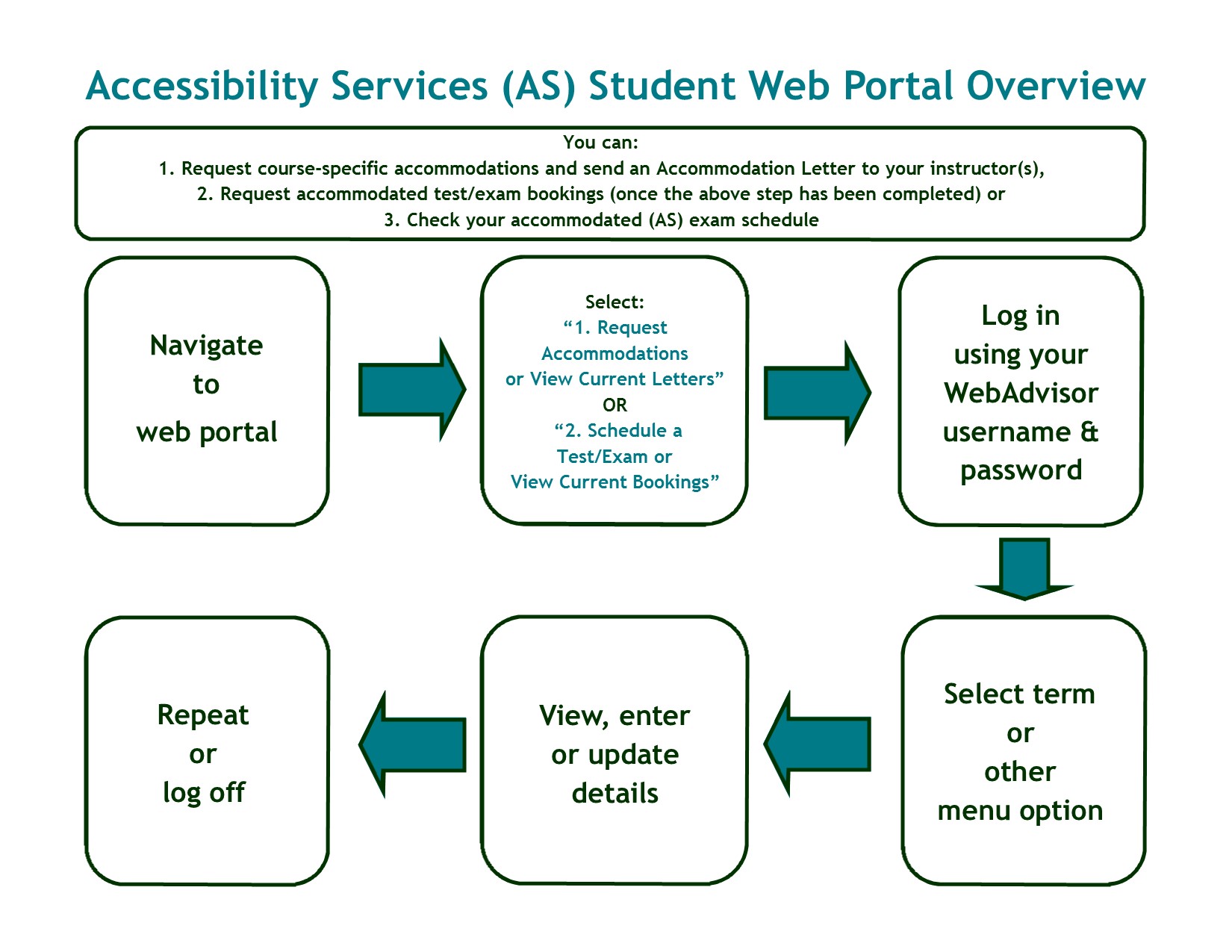
The potential of this strategy together with person center care has shown that high-risk persons with multimorbidity could be beneficiated having fewer services utilization due to complications associated with NCDs. Furthermore, it guarantees timely treatment and follow-up during transition between health services. 
The professional and collaborative process of assessing, planning, implementing, monitoring, coordinating and evaluating can be adjusted to individual requirements placing personal care on the center. Ĭase management services has shown to been essential in the approach of high-risk people with multimorbidity. This approach could potentially prevent complications of underlying diseases, reducing the use of health services and personal health costs, keeping sick people under control. Hence, the risk stratification of the Kaiser Permanente Model that segments the chronic population for a more effective care delivery organization. Therefore, integrated care comprising a comprehensive person center approach, support in clinical decision-making, self-management support, integrated health information systems, and community participation seems to be today the best approach. 
Multimorbidity is defined as the presence of two or more NCDs in a person, and it is associated with a worse quality of life, higher mortality, polypharmacy, and higher costs in health. To face this challenge in an effective way, care delivery needs to make the transition from the standard disease approach to patient-centered care with a strong emphasis on person multimorbidity and risk stratification. Moreover, the COVID-19 pandemic has changed care priorities, abruptly disrupting chronic care, probably deepening this problem. Though, putting NCDs approach as a priority in the health plan. This explosion caused by globalization, unhealthy lifestyles, and an aging population, among other things, is affecting mainly middle and high-income countries. Health systems have been challenged for the last years by the epidemic of noncommunicable diseases (NCDs), delivering in death of 41 million people each year, equivalent to 71% of all deaths globally. The Ministry of Health has taken the systematization and consolidation of the conditions for the national scale-up. We can conclude that this complex intervention was feasible to be implemented in a real context. A complete description of the high-risk intervention strategy is provided to contribute to this emerging topic and facilitate its scale-up. The training for new roles and the constant implementation support from the Centro de Innovación en Salud ANCORA UC team were essential in the progress and success of the intervention. With the proper barriers and facilitators of a real context intervention, the implementation process allowed the systematization and consolidation of the intervention provided in this study. Results showed that intervened patients had a significantly lower incidence in mortality (OR 0.56 95% CI 0.40–0.77), hospital admissions, length of stay, and the number of hospital emergency consultancies. The impact analysis was performed used generalized linear models. The studied population was 3,933 patients who belonged to similar size and location primary care centers. A cohort study was conducted with high-risk patients with multimorbidity, stratified by ACG ®, intervened between April 2017 and December 2019. This study aimed to evaluate the impact of this strategy in terms of health services utilization and mortality. In this context, Centro de Innovación en Salud ANCORA UC, together with Servicio de Salud Metropolitano Sur Oriente, implemented as a pilot study High-Risk Multimorbidity Integrated Care strategy. Interventions strategies and their implementation are still an emerging topic. During recent years, multimorbidity has taken relevance because of the impact of causes in the system, people, and their families, which has been a priority in the health care plan. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
